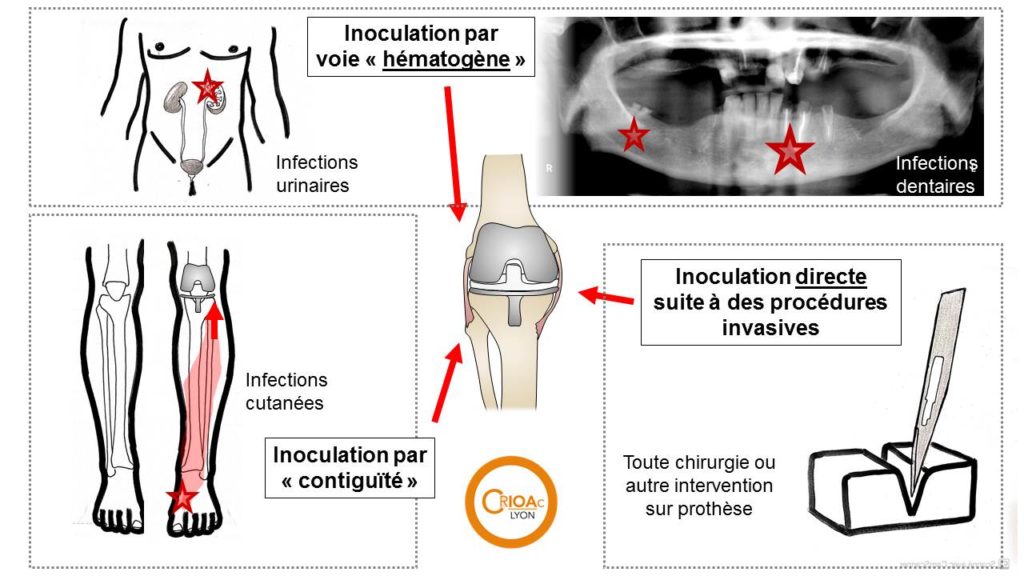
Another route of entry is direct inoculation, for example in the aftermath of a fracture or an open wound or after revision of a knee prosthesis. BJIs are often “post-operatory” infections. The risk is even greater when the patient is elderly, frail, a smoker, and has already had multiple operations. With a combination of these risk factors, the post-operative infection rate can be more than 50%. BJI can also be caused through a contiguous route, that is to say, a nearby infection can gradually contaminate bone tissue or a prosthesis. BJI can be the result of : (i) a deep and persistant skin wound, common in paraplegic patients, who have bedsores due to prolonged pressure on the skin; or (ii) a contagious skin infection such as dermo-hypodermitis or erysipelas, which can spread to a knee prosthesis.
These infections are heterogeneous because any bone or joint can be affected, any bacteria and any route (haematogenous, contiguous or post-operative) can be involved. Since treatment is most often surgical or medical, the evaluation of antibiotic treatment and different strategies is complex.
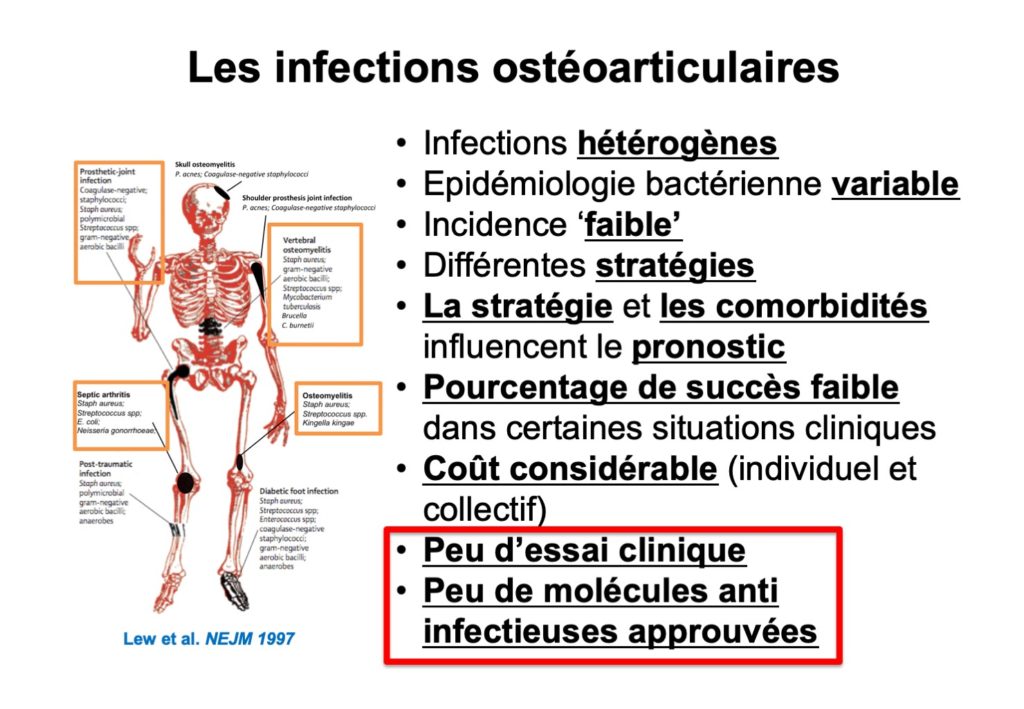
The direct and indirect cost of prosthesis infections is considerable, and greatly underestimated. The personal cost to the patient is significant due to resulting physical disability and prolonged sick-leave and hospitalisation. The social cost is also significant: for example, a BJI can cost the French public health care system 50 000 euros when superinfection occurs during a prosthesis change. Current knowledge is mainly based on experience and observation, and there are few clinical trials in the field of BJI. As a result, there are few antibiotics approved for this indication. Compared to rarer infections such as meningitis, or ones such as urinary tract infections, therapeutic trials are rare in the field of BJI. Thus, BJIs can be considered as one of the “neglected infectious diseases” of industrialised countries.



